Urinary tract infection
| Urinary tract infection | |
|---|---|
| Other names | Acute cystitis, simple cystitis, bladder infection, symptomatic bacteriuria |
Vulvovaginitis, urethritis, pelvic inflammatory disease, interstitial cystitis,[5] kidney stone disease[6] | |
| Treatment | Antibiotics (nitrofurantoin or trimethoprim/sulfamethoxazole)[7] |
| Frequency | 152 million (2015)[8] |
| Deaths | 196,500 (2015)[9] |
A urinary tract infection (UTI) is an
The most common cause of infection is
In uncomplicated cases, UTIs are treated with a short course of
About 150 million people develop a urinary tract infection in a given year.[2] They are more common in women than men, but similar between anatomies while carrying indwelling catheters.[7][18] In women, they are the most common form of bacterial infection.[19] Up to 10% of women have a urinary tract infection in a given year, and half of women have at least one infection at some point in their lifetime.[4][7] They occur most frequently between the ages of 16 and 35 years.[7] Recurrences are common.[7] Urinary tract infections have been described since ancient times with the first documented description in the Ebers Papyrus dated to c. 1550 BC.[20]
Signs and symptoms

Lower urinary tract infection is also referred to as a bladder infection. The most common symptoms are
UTIs have been associated with onset or worsening of
Children
In young children, the only symptom of a urinary tract infection (UTI) may be a fever.
Elderly
Urinary tract symptoms are frequently lacking in the elderly.[11] The presentations may be vague with incontinence, a change in mental status, or fatigue as the only symptoms,[10] while some present to a health care provider with sepsis, an infection of the blood, as the first symptoms.[7] Diagnosis can be complicated by the fact that many elderly people have preexisting incontinence or dementia.[11]
It is reasonable to obtain a urine culture in those with signs of systemic infection that may be unable to report urinary symptoms, such as when advanced dementia is present.[30] Systemic signs of infection include a fever or increase in temperature of more than 1.1 °C (2.0 °F) from usual, chills, and an increased white blood cell count.[30]
Cause
Intercourse
In young sexually active women, sexual activity is the cause of 75–90% of bladder infections, with the risk of infection related to the frequency of sex.
Sex
Women are more prone to UTIs than men because, in females, the
Chronic prostatitis in the forms of chronic prostatitis/chronic pelvic pain syndrome and chronic bacterial prostatitis (not acute bacterial prostatitis or asymptomatic inflammatory prostatitis) may cause recurrent urinary tract infections in males. Risk of infections increases as males age. While bacteria is commonly present in the urine of older males this does not appear to affect the risk of urinary tract infections.[41]
Urinary catheters
Male
Others
A predisposition for bladder infections may run in families.
Persons with spinal cord injury are at increased risk for urinary tract infection in part because of chronic use of catheter, and in part because of voiding dysfunction.[48] It is the most common cause of infection in this population, as well as the most common cause of hospitalization.[48]
Pathogenesis
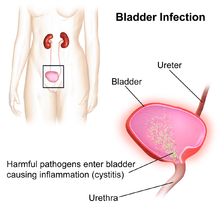
The bacteria that cause urinary tract infections typically enter the bladder via the urethra. However, infection may also occur via the blood or lymph.[7] It is believed that the bacteria are usually transmitted to the urethra from the bowel, with females at greater risk due to their anatomy.[7] After gaining entry to the bladder, E. Coli are able to attach to the bladder wall and form a biofilm that resists the body's immune response.[7]
Escherichia coli is the single most common microorganism, followed by Klebsiella and Proteus spp., to cause urinary tract infection. Klebsiella and Proteus spp., are frequently associated with stone disease. The presence of Gram positive bacteria such as Enterococcus and Staphylococcus is increased.[49]
The increased resistance of urinary pathogens to quinolone antibiotics has been reported worldwide and might be the consequence of overuse and misuse of quinolones.[49]
Diagnosis

In straightforward cases, a diagnosis may be made and treatment given based on symptoms alone without further laboratory confirmation.
Based on pH
Normal urine pH is slightly acidic, with usual values of 6.0 to 7.5, but the normal range is 4.5 to 8.0. A urine pH of 8.5 or 9.0 is indicative of a urea-splitting organism, such as Proteus, Klebsiella, or Ureaplasma urealyticum; therefore, an asymptomatic patient with a high pH means UTI regardless of the other urine test results. Alkaline pH also can signify struvite kidney stones, which are also known as "infection stones".[6]
Classification
A urinary tract infection may involve only the lower urinary tract, in which case it is known as a bladder infection. Alternatively, it may involve the upper urinary tract, in which case it is known as pyelonephritis. If the urine contains significant bacteria but there are no symptoms, the condition is known as
Children
To make the diagnosis of a urinary tract infection in children, a positive urinary culture is required. Contamination poses a frequent challenge depending on the method of collection used, thus a cutoff of 105 CFU/mL is used for a "clean-catch" mid stream sample, 104 CFU/mL is used for catheter-obtained specimens, and 102 CFU/mL is used for
Differential diagnosis
In women with
Prevention
A number of measures have not been confirmed to affect UTI frequency including: urinating immediately after intercourse, the type of underwear used, personal hygiene methods used after urinating or
Using urinary catheters as little and as short of time as possible and appropriate care of the catheter when used prevents catheter-associated urinary tract infections.[42] They should be inserted using sterile technique in hospital however non-sterile technique may be appropriate in those who self catheterize.[44] The urinary catheter set up should also be kept sealed.[44] Evidence does not support a significant decrease in risk when silver-alloy catheters are used.[59]
Medications
For those with recurrent infections, taking a short course of antibiotics when each infection occurs is associated with the lowest antibiotic use.
In cases where infections are related to intercourse, taking antibiotics afterwards may be useful.
Children
The evidence that
Dietary supplements
Some research suggests that
As of 2022[update], one review found that taking mannose was as effective as antibiotics to prevent UTIs,[73] while another review found that clinical trial quality was too low to allow any conclusion about using D‐mannose to prevent or treat UTIs.[74]
Treatment
The mainstay of treatment is antibiotics. Phenazopyridine is occasionally prescribed during the first few days in addition to antibiotics to help with the burning and urgency sometimes felt during a bladder infection.[75] However, it is not routinely recommended due to safety concerns with its use, specifically an elevated risk of methemoglobinemia (higher than normal level of methemoglobin in the blood).[76] Paracetamol may be used for fevers.[77] There is no good evidence for the use of cranberry products for treating current infections.[78][79]
Fosfomycin can be used as an effective treatment for both UTIs and complicated UTIs including acute pyelonephritis.[80] The standard regimen for complicated UTIs is an oral 3g dose administered once every 48 or 72 hours for a total of 3 doses or a 6 grams every 8 hours for 7 days to 14 days when fosfomycin is given in IV form.[80]
Uncomplicated
Uncomplicated infections can be diagnosed and treated based on symptoms alone.
Fluoroquinolones are not recommended as a first treatment.
Complicated
Complicated UTIs are more difficult to treat and usually requires more aggressive evaluation, treatment, and follow-up.[89] It may require identifying and addressing the underlying complication.[90] Increasing antibiotic resistance is causing concern about the future of treating those with complicated and recurrent UTI.[91][92][93]
Asymptomatic bacteriuria
Those who have bacteria in the urine but no symptoms should not generally be treated with antibiotics.
Pregnant women
Urinary tract infections, even asymptomatic presence of bacteria in the urine, are more concerning in pregnancy due to the increased risk of kidney infections.
Pyelonephritis
Pyelonephritis is treated more aggressively than a simple bladder infection using either a longer course of oral antibiotics or intravenous antibiotics.[3] Seven days of the oral fluoroquinolone ciprofloxacin is typically used in areas where the resistance rate is less than 10%. If the local antibiotic resistance rates are greater than 10%, a dose of intravenous ceftriaxone is often prescribed.[3] Trimethoprim/sulfamethoxazole or amoxicillin/clavulanate orally for 14 days is another reasonable option.[102] In those who exhibit more severe symptoms, admission to a hospital for ongoing antibiotics may be needed.[3] Complications such as ureteral obstruction from a kidney stone may be considered if symptoms do not improve following two or three days of treatment.[10][3]
Prognosis
With treatment, symptoms generally improve within 36 hours.[19] Up to 42% of uncomplicated infections may resolve on their own within a few days or weeks.[4][103]
15–25% of adults and children have chronic symptomatic UTIs including recurrent infections, persistent infections (infection with the same pathogen), a re-infection (new pathogen), or a relapsed infection (the same pathogen causes a new infection after it was completely gone).[74] Recurrent urinary tract infections are defined as at least two infections (episodes) in a six-month time period or three infections in twelve months, can occur in adults and in children.[74]
Cystitis refers to a urinary tract infection that involves the lower urinary tract (bladder). An upper urinary tract infection which involves the kidney is called pyelonephritis. About 10–20% of pyelonephritis will go on and develop scarring of the affected kidney. Then, 10–20% of those develop scarring will have increased risk of hypertension in later life.[104]
Epidemiology
Urinary tract infections are the most frequent bacterial infection in women.[19] They occur most frequently between the ages of 16 and 35 years, with 10% of women getting an infection yearly and more than 40–60% having an infection at some point in their lives.[7][4] Recurrences are common, with nearly half of people getting a second infection within a year. Urinary tract infections occur four times more frequently in females than males.[7] Pyelonephritis occurs between 20 and 30 times less frequently.[4] They are the most common cause of hospital-acquired infections accounting for approximately 40%.[105] Rates of asymptomatic bacteria in the urine increase with age from two to seven percent in women of child-bearing age to as high as 50% in elderly women in care homes.[39] Rates of asymptomatic bacteria in the urine among men over 75 are between 7–10%.[11] 2–10% of pregnant women have asymptomatic bacteria in the urine and higher rates are reported in women who live in some underdeveloped countries.[99]
Urinary tract infections may affect 10% of people during childhood.[7] Among children, urinary tract infections are most common in uncircumcised males less than three months of age, followed by females less than one year.[28] Estimates of frequency among children, however, vary widely. In a group of children with a fever, ranging in age between birth and two years, 2–20% were diagnosed with a UTI.[28]
History
Urinary tract infections have been described since ancient times with the first documented description in the Ebers Papyrus dated to c. 1550 BC.[20] It was described by the Egyptians as "sending forth heat from the bladder".[106] Effective treatment did not occur until the development and availability of antibiotics in the 1930s before which time herbs, bloodletting and rest were recommended.[20]
See also
References
- ^ a b c d e f "Urinary Tract Infection". Centers for Disease Control and Prevention (CDC). 17 April 2015. Archived from the original on 22 February 2016. Retrieved 9 February 2016.
- ^ PMID 25853778.
- ^ PMID 21888302.
- ^ PMID 18061019.
- ISBN 9781405103572. Archivedfrom the original on 24 April 2017.
- ^ PMID 29261874..
 Text was copied from this source, which is available under a Creative Commons Attribution 4.0 International License Archived 16 October 2017 at the Wayback Machine
Text was copied from this source, which is available under a Creative Commons Attribution 4.0 International License Archived 16 October 2017 at the Wayback Machine - ^ PMID 21349630.
- PMID 27733282.
- PMID 27733281.
- ^ PMID 21782073.
- ^ PMID 21404794.
- ISBN 9780323293181. Archivedfrom the original on 16 February 2016.
- ISBN 9781455776412. Archivedfrom the original on 11 January 2023. Retrieved 17 September 2017.
- ISBN 9780781763837. Archivedfrom the original on 16 February 2016.
- PMID 26475950.
- PMID 26475951.
- ^ PMID 24669389.
- PMID 23362450.
- ^ PMID 22010614.
- ^ ISBN 978-0-313-35009-2. Archivedfrom the original on 28 May 2016.
- ISBN 978-1-4419-7731-1. Archivedfrom the original on 10 June 2016.
- ^ S2CID 24455646.
- ^ PMID 34448496.
- PMID 24596591.
- PMID 30717706.
- ^ PMID 34711238.
- ^ PMID 35389369.
- ^ PMID 21782079.
- S2CID 195327630.
- ^ ABIM Foundation, AMDA – The Society for Post-Acute and Long-Term Care Medicine, archivedfrom the original on 13 September 2014, retrieved 20 April 2015
- PMID 26388331.
- S2CID 24123416.
- from the original on 16 March 2020. Retrieved 2 July 2019.
- S2CID 23726078.
- ^ "Urinary Tract Infections in Adults". Archived from the original on 9 January 2015. Retrieved 1 January 2015.
- PMID 20353145.
- PMID 16298166.
- ISBN 978-0-7817-5342-5.
- ^ PMID 21095409.
- PMID 25356287.
- PMID 26926816.
- ^ S2CID 40832193.
- PMID 16625600.
- ^ from the original on 16 March 2020. Retrieved 2 July 2019.
- PMID 22752741. Archived from the original on 26 May 2013. Retrieved 4 April 2013.)
{{cite journal}}: CS1 maint: unfit URL (link - ^ PMID 23152269.
The incidence of urinary tract infection (UTI) is greater in uncircumcised babies
- PMID 23201382.
- ^ S2CID 35850310.
- ^ ISBN 978-1-4443-4514-8.
- ^ PMID 26475952.
- PMID 21095410.
- ISBN 978-1-4419-6504-2. Archivedfrom the original on 20 May 2016.
- ISBN 978-0-89603-789-2. Archivedfrom the original on 4 May 2016.
- ISBN 978-1-4051-0461-6. Archivedfrom the original on 27 May 2016.
- ^ ISBN 9780781791410. Archivedfrom the original on 24 April 2016.
- ^ ISBN 9781901865639. Archivedfrom the original on 15 May 2016.
- PMID 19195972.
- PMID 25051345.
- PMID 25248140.
- ISBN 9780781771559. Archivedfrom the original on 9 June 2016.
- from the original on 20 January 2023. Retrieved 20 January 2023.
- PMID 35264408.
- ^ PMID 27092529.
- ^ PMID 18425910.
- PMID 23757735.
- PMID 30093359.
- PMID 29803843.
- S2CID 6714180.
- S2CID 41304559.
- PMID 22777630.
- PMID 37947276.
- PMID 26695595.
- PMID 32497610.
- ^ PMID 36041061.
- PMID 15311491.
- ISBN 978-0-444-53273-2. Archivedfrom the original on 7 May 2016.
- ISBN 978-0-8261-1812-7. Archivedfrom the original on 11 June 2016.
- PMID 17315052.
- S2CID 26916844.
- ^ PMID 32300381.
- PMID 25335150.
- ^ PMID 20927755.
- ^ "FDA Drug Safety Communication: FDA updates warnings for oral and injectable fluoroquinolone antibiotics due to disabling side effects". Food and Drug Administration (FDA). 8 March 2018. Archived from the original on 18 July 2019. Retrieved 17 July 2019.
- .
- ^ PMID 21292654.
- ABIM Foundation, American Urogynecologic Society, archivedfrom the original on 2 June 2015, retrieved 1 June 2015
- PMID 22516128.
- ^ Afzalnia S (15 December 2006). "BestBets: Is a short course of antibiotics better than a long course in the treatment of UTI in children". www.bestbets.org. Archived from the original on 14 August 2009.
- ISBN 978-0-7216-9056-8. Archivedfrom the original on 13 February 2012.
- PMID 23538307.
- PMID 20876625.
- PMID 23809723.
- PMID 29750894.
- PMID 22003486.
- PMID 17002033.
- ^ a b American Geriatrics Society, "Five Things Physicians and Patients Should Question", Choosing Wisely: an initiative of the ABIM Foundation, American Geriatrics Society, archived from the original on 1 September 2013, retrieved 1 August 2013
- PMID 26560337.
- ^ PMID 20824868.
- ^ PMID 31765489.
- PMID 24251228.
- ^ PMID 26221993.
- ISBN 978-1-930808-65-2.
- S2CID 52942247.
- S2CID 22331470.
- ISBN 978-0-7817-8589-1. Archivedfrom the original on 28 April 2016.
- ISBN 978-0-7131-4591-5.
